Drs. Wong and Borno are assistant professors of pharmacy practice at Arnold and Marie Schwartz College of Pharmacy and Health Sciences, Long Island University, Brooklyn, New York.
Bacteria can cause different types of skin infections. Three common skin infections that you and your doctor may encounter are: (1) cellulitis, (2) folliculitis, and (3) impetigo. Keep in mind that skin infections vary in presentation and treatment. Therefore, it is important to talk to your doctor to obtain an appropriate diagnosis and treatment plan.
Cellulitis
Cellulitis is an infection that involves the outer layers of the skin. It is commonly caused by bacteria known as beta-hemolytic streptococcus or Staphylococcus aureus. You may experience pain, swelling, tenderness, warmth, and redness in the infected area. If you have a severe case of cellulitis, you may experience fever, tiredness, and a lowering of blood pressure. If left untreated, pus may form and cells may die in the infected skin area. Cellulitis can involve any part of the body but most often affects the leg. It typically results from an injury to the skin, such as scratches or animal bites—these allow bacteria to enter the body and cause an infection. An additional cause of cellulitis is skin breakdown around the anal area, typically seen in children. This can lead to redness, swelling, and painful bowel movements.
Oral antibiotics are used to treat mild cellulitis; more severe cases must be treated with intravenous antibiotics in a hospital. Antibiotics that may be used include cephalosporins, dicloxacillin, clindamycin, or vancomycin. Swelling can be lessened by elevating the affected area, such as the legs or arms. To stop cellulitis from occurring again, it is important to keep applying lotion to the skin and to maintain good skin cleanliness.
Folliculitis
Folliculitis is a general term used to describe an infection of the hair follicles commonly caused by Staphylococcus aureus, resulting in red pimples. You may experience redness, tenderness, or swelling of the affected area. It also can spread to the deeper parts of the hair follicles and pus can form, also known as furuncles or boils. Carbuncles is a term used to describe a group of infected hair follicles. Folliculitis, furuncles, and carbuncles can be seen on any part of the body with hair, such as the face, scalp, thighs, underarms, and groin area. This includes areas that are bearded or shaved.
Mild folliculitis can be treated with topical antibiotics, such as erythromycin, clindamycin, or mupirocin. More severe infections, such as carbuncles and larger furuncles, may require a surgical cut and drainage of the affected area. After drainage, it is important to clean the area with antibacterial soap; then you should apply the antibiotic ointment to the affected area of the skin. If needed, your doctor may prescribe oral antibiotics such as cephalosporins or dicloxacillin. Keep in mind that your doctor may recommend monthly treatments with mupirocin ointment if you have folliculitis that occurs repeatedly.
Impetigo
Impetigo is a contagious skin infection commonly caused by Staphylococcus aureus. Although this infection may occur in adults, it is most often seen in children aged 2 to 5 years and is usually spread through direct contact with another person who has the infection. You may experience tenderness, itching, sores, or blisters that can rupture and form honey-colored crusts. It can affect different parts of the body such as the face, arms, or legs. It also can affect moist parts of the body, such as the armpits, neck folds, and diaper areas.
Impetigo can be treated with a topical ointment or oral antibiotic. Mupirocin is a typical ointment that may be prescribed by your doctor. Oral antibiotics such as penicillins or cephalosporins are used for more severe infections. To prevent the spread of the infection to other parts of the body, avoid scratching the blisters or sores. Because impetigo is commonly seen in children, it may be helpful to cut the fingernails and cover the affected areas of the body with bandages or gauze. It also is important to prevent the spread of infection to other individuals in close contact by not sharing things such as blankets, linens, toys, or clothing.
What about MRSA Infections?
MRSA stands for methicillin-resistant Staphylococcus aureus. It is a form of Staphylococcus aureus or “staph” bacteria that is resistant to certain antibiotics. It is transmitted by directly contacting an infected person, touching contaminated surfaces, or sharing personal items that have been in contact with infected skin. MRSA is a large problem in hospitals or health care facilities (like dialysis centers and nursing homes). MRSA also can infect people in the community, however, such as children at day care centers and children who are involved in sports that involve close contact. This is known as community-associated MRSA or CA-MRSA.
MRSA infections can appear like a pimple or boil, with redness, swelling, pain, or pus. Serious infections may spread into the blood and cause blood infections. If you experience a MRSA infection, your doctor may drain the infected area and prescribe antibiotics such as linezolid, clindamycin, or doxycycline. Do not try to drain the wound yourself! This can worsen the infection or spread it to others.
To prevent the spread of MRSA, here are some helpful tips:
- Cover your wound with clean, dry bandages until the affected area is completely healed.
- Maintain good hand hygiene—you and those in close contact with you should wash hands frequently with soap and water.
- Do not share personal items, such as linens and clothing, with others.
General Management of Skin Infections
With antibiotic treatment, signs and symptoms of skin infections begin to improve after approximately 2 to 3 days. If your skin infection does not improve or gets worse (especially if you develop a fever or the infection spreads), notify your doctor right away. If you are prescribed topical or oral antibiotics, be sure to finish the full course of antibiotics unless otherwise directed. Keep in mind that the length of treatment will differ depending on the type and severity of the infection. Lastly, as is true among all skin infections, you should keep the affected area or wound clean with good skin hygiene.
Join the Community
There are several types of treatment for skin fungus, ranging from home remedies to treatment from a doctor. Though it is often possible to treat skin infections at home, patients are still advised to see a doctor first for a proper diagnosis, because skin fungus can be confused with other conditions. A visit to the doctor usually results in a prescription antifungal cream or tablet that can get rid of the issue. Patients often can find over-the-counter treatments, including medicated spray, powder and shampoo. Home remedies used to treat skin fungus usually include vinegar, hydrogen peroxide and tea tree oil.
Vinegar can be used topically to treat skin fungus.
Patients are often advised to see a doctor when they suspect skin fungus, because this allows them to be properly diagnosed and treated with prescription medication, if necessary. Doctors often take the symptoms and appearance of the skin into account, and may perform a culture before making a diagnosis. Once the diagnosis is made, the doctor will likely prescribe antifungal cream, a pill or shampoo, depending on where the fungus is on the skin. Prescription medications are often stronger and more effective than over-the-counter kinds, but they may have side effects, such as an upset stomach. Patients should report to their doctor if the skin irritation does not appear to be clearing up with proper use of the medication, as well as if they notice any side effects.
It is possible to get treatment for skin fungus without a prescription, and many drugstores sell products that can eliminate the issue. Patients can typically buy sprays, shampoos and creams without a prescription, though these tend to take longer to work than prescription medications. One example of a common over-the-counter treatment is tolnaftate, which is often used to treat athlete’s foot, while clotrimazole is typically used to treat ringworm and jock itch. Patients also can buy hydrocortisone cream to relieve the itch while they wait for the antifungal products to get rid of the infection.
Tolnaftate is often used to treat athlete’s foot, a type of skin fungus.
Some patients prefer not to use modern medicine, and would rather try simple remedies using products they have at home. For example, soaking the affected area in a mixture of hydrogen peroxide and water often works as a simple home treatment for skin fungus. The same can be done with vinegar up to three times a day, though patients are advised to wash off the mixture when they are done soaking to avoid smelling the strong odor of vinegar all day. Tea tree oil is another treatment for skin fungus that can be used at home, and applying this liquid to the affected area with a dropper twice a day should clear up the infection.
Many antifungal creams contain the steroid hydrocortisone to help relieve itching.
In this Article
In this Article
In this Article
- Self-Care at Home
- Medical Treatment
Self-Care at Home
Most candidal (yeast) infections can be treated at home with over-the-counter or prescription medication and will clear up within a week. If some other disease has weakened a person’s immune system, the person should consult a doctor about any new symptoms before attempting self-treatment because of the risk of infection.
- Vaginal yeast infections
- Most women can treat vaginal yeast infections at home with nonprescription vaginal creams or suppositories.
- A single dose of fluconazole (Diflucan) tablet also cures most vaginal yeast infections. Fluconazole requires a prescription from your physician.
- Thrush
- For thrush, swish the antifungal agent nystatin around in your mouth then swallow the liquid. Take care to maintain excellent oral hygiene.
- All objects put into a child’s mouth should be washed or sterilized after each use.
- Breastfeeding mothers should be evaluated for Candida infection of the breast.
- If you wear dentures, clean them thoroughly after each use and practice good oral hygiene.
- Adults and older children have several treatment options not available to babies, such as troches (antifungal lozenges) or pills such as fluconazole (Diflucan) to help clear the infection in addition to nystatin.
- Skin and diaper rash
- Clotrimazole (Lotrimin) creams and lotions can be applied to superficial skin infections. Other medications require a prescription and a visit to your doctor.
- Other antifungal creams, such as ketoconazole (Nizoral), which is available by prescription, is helpful as well.
- For paronychia, a skin rash around the nails, avoiding moisture can be helpful. Oral itraconazole (Sporanox) or fluconazole (Diflucan) can also be helpful and can be prescribed by a doctor. Topical antifungal and topical corticosteroids are also used.
- PerlГЁche is treated with topical antiyeast or antifungal agents, and often with a mild corticosteroid cream. Limit lip licking of the corners of the mouth. Placing a bit of petroleum jelly on top of the antiyeast agents can be helpful as well.
- The affected area should be kept clean and dry.
- For diaper rashes, frequent diaper changes and the use of barrier creams speed recovery .
- Intertrigo can benefit from the use of nystatin powder, which decreases the amount of moisture and also acts as an antiyeast agent.
Continued
Medical Treatment
A wide array of treatment options is available to treat candidiasis. Options include creams, lotions, tablets or capsules, troches (lozenges), and vaginal suppositories or creams. Talk to your doctor to find the option that is right for you.
- Azole medications are a family of antifungal drugs that end in the suffix “-azole.” They block the manufacture of ergosterol, a crucial material of the yeast cell wall. Without ergosterol, the yeast cell wall becomes leaky and the yeast die. Fortunately, ergosterol is not a component of human membranes, and azoles do not harm human cells.
- Polyene antifungal medications include nystatin and amphotericin B. Nystatin is used for thrush and superficial candidal infections. Doctors reserve amphotericin B for more serious systemic fungal infections. The antifungals work by attaching to the yeast cell wall building material, ergosterol. These medications then form artificial holes in the yeast wall that cause the yeast to leak and die.
Medically reviewed by Drugs.com. Last updated on Feb 3, 2020.
- Overview
- Aftercare Instructions
- Ambulatory Care
- En Español
WHAT YOU NEED TO KNOW:
What do I need to know about a skin yeast infection?
Yeast is normally present on the skin. Infection happens when you have too much yeast, or when it gets into a cut on your skin. Certain types of mold and fungus can cause a yeast infection. A skin yeast infection can appear anywhere on your skin or nail beds. Skin yeast infections are usually found on warm, moist parts of the body. Examples include between skin folds or under the breasts.
What increases my risk for a skin yeast infection?
- Elderly age, especially as skin gets thinner and tears more easily
- Obesity that causes skin folds where moisture can collect
- Diapers that are not changed regularly and allow moisture to sit on your baby’s skin
- Diabetes, especially if it is not controlled
- Bedrest that allows moisture to collect on your skin
- Immune system problems
- Certain medicines, including antibiotics or medicines that weaken your immune system
- Pregnancy or hormone changes
- Moisture left on your feet or between your toes after you bathe, or that builds up under a ring you wear
What are the signs and symptoms of a skin yeast infection?
Signs and symptoms will depend on the type of yeast causing the infection, and where the infection is located.
- Red, scaly skin
- Changes in skin color, especially a beefy red color
- Itching, dry skin
- Painful, cracking skin at the corners of your mouth
- Thick, discolored, chipping nails
- Skin lesions that may be red or purple and round
- Pus bumps
How is a skin yeast infection diagnosed and treated?
Your healthcare provider may know you have a skin yeast infection from your signs and symptoms. He may take a sample of your skin to check for fungus. He may also look at areas of your skin under ultraviolet light to show which type of yeast infection you have. You may be given an antifungal cream or ointment to treat the infection. You may be given antifungal medicine as a pill if your infection is severe.
How do I care for the skin near the infection?
You may only have discolored patches of skin, or areas that are dry and flaking. Care for these skin problems as directed by your healthcare provider. If you have painful skin or an open sore, you will need to protect the skin and prevent damage. You will also need to keep the skin dry as much as possible. Ask your healthcare provider how to care for your skin while the infection clears. The following are general guidelines for caring for painful or open skin:
- Keep the skin clean. Ask your healthcare provider if you should wash with mild soap and water. Do not use soap that contains alcohol. Alcohol can dry and irritate the skin and make symptoms worse. Your baby’s healthcare provider may tell you to use diaper cream or ointment when you change his diaper. This will protect the skin and prevent moisture from collecting.
- Keep the skin dry. Pat the area dry with a towel. Do not rub, because this may irritate the skin. If you have a skin yeast infection between skin folds, lift the top part gently and hold it while you dry between your skin folds. Always dry your feet completely after you swim or bathe, including between your toes. Dry your skin if you are sweating from exercise or exposure to heat. Use a clean towel each time to prevent spreading or continuing the infection.
- Keep the skin protected. Ask your healthcare provider if you should cover the area with a bandage or leave it open. Check your skin each day to make sure you do not have new or worsening problems. You may need to have someone check the skin if you cannot see the area easily.
What can I do to prevent a skin yeast infection?
- Do not share clothing or towels
- Wear shower shoes if you need to use a public shower
- Dry your feet completely after you bathe, and apply antifungal powder or cream as directed
- Put on socks before you get dressed so you do not spread fungus from your feet
- Wear light clothing that allows air to get to your skin
- Manage your weight to prevent skin folds where yeast can collect
- Manage diabetes
- Change your baby’s diaper often, and keep the area clean and dry as much as possible
- Use a diaper cream or ointment that contains zinc oxide or dimethicone on your baby’s diaper area as directed
When should I seek immediate care?
- You have signs of infection, such as pus, warmth or red streaks coming from the wound, or a fever.
When should I contact my healthcare provider?
- Your symptoms worsen or do not get better within 7 to 10 days.
- You have new or returning signs of a skin yeast infection after treatment.
- You have questions or concerns about your condition or care.
Care Agreement
© Copyright IBM Corporation 2020 Information is for End User’s use only and may not be sold, redistributed or otherwise used for commercial purposes. All illustrations and images included in CareNotes® are the copyrighted property of A.D.A.M., Inc. or IBM Watson Health
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
Although there are millions of species of fungi, only about 300 of them can actually cause infections in humans. There are several types of fungal infections that can affect your skin.
In this article, we’ll take a closer look at some of the most common fungal skin infections and the ways they can be treated and prevented.
Fungi live everywhere. They can be found in plants, soil, and even on your skin. These microscopic organisms on your skin typically don’t cause any problem, unless they multiply faster than normal or penetrate your skin through a cut or lesion.
Since fungi thrive in warm, moist environments, fungal skin infections can often develop in sweaty or damp areas that don’t get much airflow. Some examples include the feet, groin, and folds of skin.
Often, these infections appear as a scaly rash or discoloration of the skin that is often itchy.
Some fungal skin infections are very common. Although the infection can be annoying and uncomfortable, it’s typically not serious.
Fungal skin infections are often spread through direct contact. This can include coming into contact with fungi on clothing or other items, or on a person or animal.
Many common fungal infections can affect the skin. In addition to the skin, another common area for fungal infections is mucous membranes. Some examples of these are vaginal yeast infections and oral thrush.
Below, we’ll explore some of the most common types of fungal infections that can impact the skin.
Ringworm of the body (tinea corporis)
Contrary to its name, ringworm is caused by a fungus and not a worm. It typically occurs on the torso and limbs. Ringworm on other areas of the body can have different names, such as athlete’s foot and jock itch.
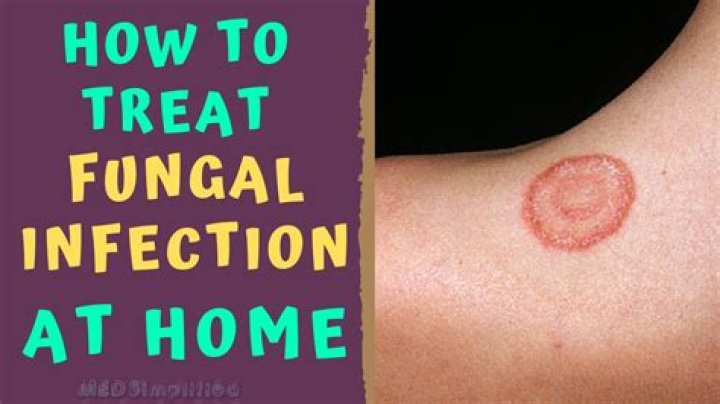
The main symptom of ringworm is a ring-shaped rash with slightly raised edges. The skin inside these circular rashes usually looks healthy. The rash can spread and is often itchy.
Ringworm is a common fungal skin infection and is highly contagious. It’s not serious, though, and can usually be treated with an antifungal cream.
Athlete’s foot (tinea pedis)
Athlete’s foot is a fungal infection that affects the skin on your feet, often between your toes. Typical symptoms of athlete’s foot include:
- itching, or a burning, stinging sensation between your toes or on the soles of your feet
- skin that appears red, scaly, dry, or flaky
- cracked or blistered skin
In some cases, the infection can also spread to other areas of your body. Examples include your nails, groin, or hands (tinea manuum).
Jock itch (tinea cruris)
Jock itch is a fungal skin infection that happens in the area of your groin and thighs. It’s most common in men and adolescent boys.
The main symptom is an itchy red rash that typically starts in the groin area or around the upper inner thighs. The rash may get worse after exercise or other physical activity and can spread to the buttocks and abdomen.
The affected skin may also appear scaly, flaky, or cracked. The outer border of the rash can be slightly raised and darker.
Ringworm of the scalp (tinea capitis)
This fungal infection affects the skin of the scalp and the associated hair shafts. It’s most common in young children and needs to be treated with prescription oral medication as well as antifungal shampoo. The symptoms can include:
- localized bald patches that may appear scaly or red
- associated scaling and itching
- associated tenderness or pain in the patches
Tinea versicolor
Tinea versicolor, sometimes called pityriasis versicolor, is a fungal/yeast skin infection that causes small oval discolored patches to develop on the skin. It’s caused by an overgrowth of a specific type of fungus called Malassezia, which is naturally present on the skin of about 90 percent of adults.
These discolored skin patches most often occur on the back, chest, and upper arms. They may look lighter or darker than the rest of your skin, and can be red, pink, tan, or brown. These patches can be itchy, flaky, or scaly.
Tinea versicolor is more likely during the summer or in areas with a warm, wet climate. The condition can sometimes return following treatment.
Cutaneous candidiasis
This is a skin infection that’s caused by Candida fungi. This type of fungi is naturally present on and inside our bodies. When it overgrows, an infection can happen.
Candida skin infections occur in areas that are warm, moist, and poorly ventilated. Some examples of typical areas that can be affected include under the breasts and in the folds of the buttocks, such as in diaper rash.
The symptoms of a Candida infection of the skin can include:
- a red rash
- itching
- small red pustules
Onychomycosis (tinea unguium)
Onychomycosis is a fungal infection of your nails. It can affect the fingernails or the toenails, although infections of the toenails are more common.
You may have onychomycosis if you have nails that are:
- discolored, typically yellow, brown, or white
- brittle or break easily
- thickened
Prescription medications are often required to treat this type of infection. In severe cases, your doctor may remove some or all of an affected nail.
What is cellulitis?
Cellulitis is a type of bacterial infection that can quickly become serious. It affects your skin, causing inflammation, redness, and pain.
This type of infection occurs when bacteria enters your body through broken skin. It can affect any part of the body, but it’s most common on the lower legs. This is because the lower legs tend to be most susceptible to scrapes and cuts.
Several types of cuts and injuries can allow cellulitis-causing bacteria into the body, including:
- surgical incisions
- burns
- puncture wounds
- skin rashes, such as severe eczema
- animal bites
A cellulitis infection can spread to your bloodstream, which can quickly become life-threatening. This is why it’s best to see a doctor as soon as possible if you think you might have cellulitis.
You shouldn’t try to treat cellulitis at home, but there are a few things you can do on your own as you recover from a cellulitis infection.
Cellulitis tends to progress quickly, so early identification is key. At first, you might just feel some pain and tenderness.
But over the course of a few hours, you may start to notice:
- skin that’s warm to the touch
- blistering
- skin dimpling
- growing area of redness
You can monitor the progression of your infection by circling the red area with a pen. This will help you see how much it’s spread within a period of time. If it’s growing, it’s time to head to the doctor. You should also seek immediate treatment if you develop any flu-like symptoms, including a fever or chills.
Treating cellulitis depends on how severe the infection is. If you have symptoms of cellulitis but no fever, you can make an appointment with your primary care doctor, as long as they’re able to see you within one day. But if you do have a fever in addition to other cellulitis symptoms, it’s best to head to the emergency room or an urgent care center.
A doctor will start by checking your symptoms. They’ll look for red, blotchy areas of skin that feel warm to the touch. If the infection seems to be in its early stages, you’ll likely just need a round of oral antibiotics. Make sure to take the full course as prescribed by your doctor, even if you stop noticing symptoms after a day or two.
Sometimes, oral antibiotics don’t work as expected, so make sure to follow up with your doctor if you aren’t noticing any improvement after two or three days. You may need a different type of antibiotic.
If the infection is spreading or seems more severe, you may need intravenous antibiotics. Your doctor may also recommend this if you have a condition that affects your immune system. Depending on your symptoms, you may need to stay in the hospital for a few days to ensure the infection doesn’t enter your bloodstream.
Sometimes oral antibiotics don’t work as well as they should. If your cellulitis is not improving after two or three days, your doctor may prescribe a different antibiotic or have you admitted for IV treatment.
Cellulitis requires treatment with antibiotics, which are only prescribed by a doctor. But as you recover at home, there are several things you can do to ease any discomfort and avoid complications.
- Covering your wound. Properly covering the affected skin will help it heal and prevent irritation. Follow your doctor’s instructions for dressing your wound and be sure to change your bandage regularly.
- Keeping the area clean. Follow your doctor’s recommendations for cleaning the affected skin.
- Elevating the affected area. If your leg is affected, lie down and elevate your leg above your heart. This will help reduce swelling and ease your pain.
- Applying a cool compress. If the affected skin is hot and painful, apply a clean washcloth soaked in cool water. Avoid chemical icepacks, as these can further irritate damaged skin.
- Taking an over-the-counter pain reliever. A nonsteroidal anti-inflammatory, like ibuprofen (Advil, Motrin) or naproxen (Aleve), can help reduce pain and inflammation.
- Treating any underlying conditions. Treat any underlying conditions, such as athlete’s foot or eczema, that caused the wound that got infected.
- Taking all your antibiotics. With antibiotic treatment, the symptoms of cellulitis should begin to disappear within 48 hours, but it’s very important to continue taking your antibiotics until all the pills are gone. Otherwise, it may come back, and the second course of antibiotics may not be as effective as the first.
Without antibiotic treatment, cellulitis can spread beyond the skin. It can enter your lymph nodes and spread into your bloodstream. Once it reaches your bloodstream, bacteria can cause quickly cause a life-threatening infection known as blood poisoning.
Without proper treatment, cellulitis can also return. Repeated cellulitis can cause permanent damage to your lymph nodes, which play an important role in your immune system.
In rare cases, severe cellulitis infections can spread into deep layers of tissue. An infection of the fascia, a deep layer of tissue surrounding your muscles and organs, is known as necrotizing fasciitis, or flesh-eating disease. People with necrotizing fasciitis usually need multiple surgeries to remove dead tissue, often entire limbs.
Cellulitis is a serious condition that shouldn’t be treated at home. Within hours, it can escalate into a life-threatening blood infection. Go to your local urgent care clinic or emergency room if you think you have cellulitis. Early antibiotic treatment is key in reducing your risk of serious complications.
Last medically reviewed on October 29, 2018
A staph infection is a type of skin infection that occurs by bacteria penetrating the skin or nose and may eventually affect internal organs. It is caused by staphylococcus bacteria and can result in many diseases such as food poisoning, toxic shock syndrome, boils, impetigo, and cellulitis. If left untreated, a staph infection may develop into methicillin-resistant Staphylococcus aureus, or MRSA, which can become deadly as it is resistant to the antibiotic methicillin and other drugs in this category. Being aware of the causes, symptoms, and treatments of a staph infection may be helpful for the prevention of one.
A staph infection may be treated with antibiotics. A medical professional may want to drain the infection through a surgical procedure in which an incisor is inserted into the infection and drained of pus.
10. Causes
© Ruslan Nassyrov | Dreamstime Stock Photos
Staph bacteria are found all over the place, including on the human body in the nostrils and skin folds. A staph infection occurs when staph bacteria penetrate the skin or nose and become infected and inflamed. Research shows that up to forty percent of healthy people are carriers of staph bacteria and many of these people show no signs or symptoms of a disease. It is not until staph bacteria penetrate the skin that an infection or symptoms occur.
9. Staph Bacteria Are Contagious
© Skypixel | Dreamstime Stock Photos
Staph bacteria are contagious and can be transmitted through contact with the bacteria, such as touching an infected object like a pillow or towel, or through contact with an infected person. Sneezing, coughing, and playing sports can spread the bacteria. Eating contaminated food may occur when food is not properly stored or has been handled by a carrier of the bacteria. A staph infection also may arise in the form of toxic shock syndrome in menstruating women who use do not regularly change tampons.
8. Risk Factors
Although a staph infection may occur in anyone, some people are more likely to develop one than others. A lack of dietary iron may result in a staph infection as iron may cause dry and brittle skin that is more susceptible to cuts and wounds where bacteria can quickly enter the bloodstream. People with a weakened immune system and those who have stayed at a hospital are more prone to developing an infection. Alcoholism may result in malabsorption, which prevents the intestines from properly absorbing food. This results in a nutritional deficiency and depletes the skin of zinc and vitamins A, B1, B2, and B3, which are needed for healthy skin.
7. Symptoms
© Smileitsmccheeze | Dreamstime Stock Photos
There are two types of staph infections: skin and invasive infections. Symptoms are associated with different diseases and depend on the kind of infection. They can start out slow or progress very quickly, while others suddenly become life-threatening. Symptoms of invasive staph infections occur when bacteria has entered internal organs. They can be deadly if left untreated. Complications of an invasive infection may include pneumonia, sepsis, and endocarditis; however, the risk of developing an invasive infection is much lower than a skin infection.
6. Boils
Boils are one of the most common symptoms of a staph infection. They occur when staph bacteria enter the skin by traveling down oil glands or hair follicles. When white blood cells begin to fight the infection, the area of the skin where the bacteria entered becomes blocked due to the overgrowth of pus, which is a mixture of protein, white blood cells, and bacteria, causing a boil to develop. Fever and tenderness may accompany it and the boil may also become swollen and red.
5. Cellulitis And Impetigo
Cellulitis is a condition that occurs when staph bacteria enter the skin through a crack and causes red patches that grow over time. Similar symptoms may include swelling, warmth, blisters, and tenderness of the skin. Impetigo occurs when small groups of blisters and yellow-colored crusty erosions called school sores develop on the hands and face. Impetigo occurs more frequently in young children but may also develop in adults with a weakened immune system.
4. Folliculitis
About Kids Health
Another symptom of a staph infection is folliculitis, which occurs when a hair follicle becomes inflamed. It may occur anywhere on the body where there is a large area of hair, such as on the scalp, chest, buttocks, arms or legs. Symptoms may include red, swollen spots with a hair in the center. These spots may become infected and develop pus that breaks open and drains, which can cause the infection to spread to other areas of the body.
3. Wound Infections
Wound infections are an indication of a staph infection. They occur when staph bacteria invade fresh wound and worsen conditions. Symptoms may include swelling, pus, and redness of the skin. Staphylococcal Scalded Skin Syndrome or SSSS may occur as a result of a staph infection. Skin irritability and fever characterize SSS. A rash that looks like a scald or burn may develop over time. Other symptoms include wrinkly or peeling skin followed by blistering.
2. Treatment
Seek treatment at the first sign of a staph infection to prevent the development of MRSA, which is an infection that no longer responds to antibiotics and can be deadly. Because it is a bacterial infection, a staph infection may be treated with antibiotics. A medical professional may want to drain the infection through a surgical procedure in which an incisor is inserted into the infection and drained of pus. Other surgical procedures may include removal of the source of infection such as heart valves, pacemakers, artificial grafts, and intravenous lines.
1. Natural Remedies
© Amarosy | Dreamstime Stock Photos
Tea tree oil contains antiseptic, antibacterial and anti-inflammatory properties to kill staph bacteria. To use, apply a few drops of tea tree oil to a cotton ball and dab the infected area. Raw, unfiltered apple cider vinegar has antibacterial and anti-inflammatory properties that can be used to kill staph bacteria. Take two tablespoons of apple cider vinegar orally twice a day or mix with water. A study published in the Journal of Microbiological Methods found that basil essential oil is effective in treating antibiotic-resistant forms of staph infections. It can be dabbed directly on the infection and added to the diet.
Medically reviewed by Drugs.com. Last updated on Feb 3, 2020.
- Overview
- Aftercare Instructions
- Ambulatory Care
- Discharge Care
- Inpatient Care
- En Español
WHAT YOU NEED TO KNOW:
What is a wound infection?
A wound infection occurs when bacteria enters a break in the skin. The infection may involve just the skin, or affect deeper tissues or organs close to the wound.
What increases my risk for a wound infection?
Anything that decreases your body’s ability to heal wounds may put you at risk for a wound infection. This includes any of the following:
- Age older than 65
- Smoking or being overweight
- Medical conditions that weaken the immune system such as diabetes, HIV, or cancer
- Medicines that cause a weak immune system such as steroids
- Radiation, chemotherapy, or poor nutrition
- Foreign objects in the wound such as glass or metal
- Decreased blood flow to the wound caused by high blood pressure, or blocked or narrowed blood vessels
What are the signs and symptoms of a wound infection?
Your symptoms may start a few days after you get the wound, or may not occur for a month or two after the wound happens:
- Fever
- Warm, red, painful, or swollen skin near the wound
- Blood or pus coming from the wound
- A foul odor coming from the wound
How is a wound infection diagnosed?
Your healthcare provider will ask about your medical history and examine you. He will ask how and when you were wounded. You may have any of the following tests:
- Blood tests may be done to check for infection.
- X-ray or CT may be done to look for infection in deep tissues or a foreign object in your wound. You may be given contrast liquid to help the pictures show up better. Tell the healthcare provider if you have ever had an allergic reaction to contrast liquid.
- A wound culture is a sample of fluid or tissue that taken from the wound. It is sent to a lab and tested for the germ that is causing the infection.
How is a wound infection treated?
Treatment will depend on how severe the wound is, its location, and whether other areas are affected. It may also depend on your health and the length of time you have had the wound. Ask your healthcare provider about these and other treatments you may need:
- Medicine will be given to treat the infection and decrease pain and swelling.
- Wound care may be done to clean your wound and help it heal. A wound vacuum may also be placed over your wound to help it heal.
- Hyperbaric oxygen therapy (HBO) may be used to get more oxygen to your tissues to help them heal. The pressurized oxygen is given as you sit in a pressure chamber.
- Surgery may be needed to clean the wound or remove infected or dead tissue. Surgery may also be needed to remove a foreign object.
How can I help my wound heal?
- Care for your wound as directed. Keep your wound clean and dry. You may need to cover your wound when you bathe so it does not get wet. Clean your wound as directed with soap and water or wound cleaner. Put on new, clean bandages as directed. Change your bandages when they get wet or dirty.
- Eat a variety of healthy foods. Examples include fruits, vegetables, whole-grain breads, low-fat dairy products, beans, lean meats, and fish. Healthy foods may help you heal faster. You may also need to take vitamins and minerals. Ask if you need to be on a special diet.
- Manage other health conditions. Follow your healthcare provider’s directions to manage health conditions that can cause slow wound healing. Examples include high blood pressure and diabetes.
- Do not smoke. Nicotine and other chemicals in cigarettes and cigars can cause slow wound healing. Ask your healthcare provider for information if you currently smoke and need help to quit. E-cigarettes or smokeless tobacco still contain nicotine. Talk to your healthcare provider before you use these products.
When should I seek immediate care?
- You feel short of breath.
- Your heart is beating faster than usual.
- You feel confused.
- Blood soaks through your bandages.
- Your wound comes apart or feels like it is ripping.
- You have severe pain.
- You see red streaks coming from the infected area.
When should I contact my healthcare provider?
- You have a fever or chills.
- You have more pain, redness, or swelling near your wound.
- Your symptoms do not improve.
- The skin around your wound feels numb.
- You have questions or concerns about your condition or care.
Care Agreement
© Copyright IBM Corporation 2020 Information is for End User’s use only and may not be sold, redistributed or otherwise used for commercial purposes. All illustrations and images included in CareNotes® are the copyrighted property of A.D.A.M., Inc. or IBM Watson Health
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
It’s a scary sight when your child comes home from day care or elementary school with red sores and oozing fluid-filled blisters. Don’t be alarmed if it’s impetigo. Impetigo — one of the most common childhood diseases — can be treated with medications approved by the U.S. Food and Drug Administration (FDA).
Impetigo is a common bacterial skin infection that can produce blisters or sores anywhere on the body, but usually on the face (around the nose and mouth), neck, hands, and diaper area. It’s contagious, preventable, and manageable with antibiotics, says pediatrician Thomas D. Smith, MD, of FDA.
What Causes Impetigo
Two types of bacteria found on our skin cause impetigo: Staphylococcus aureus and Streptococcus pyogenes (which also causes strep throat). Most of us go about our lives carrying around these bacteria without a problem, Smith says. But then a minor cut, scrape or insect bite allows the bacteria to cause an infection, resulting in impetigo.
Anyone can get impetigo — and more than once, Smith says. Although impetigo is a year-round disease, it occurs most often during the warm weather months. There are more than 3 million cases of impetigo in the United States every year.
“We typically see impetigo with kids 2 to 6 years old, probably because they get more cuts and scrapes and scratch more. And that spreads the bacteria,” Smith says.
Treating Impetigo
Look for these signs of impetigo:
- itchy red sores that fill with fluid and then burst open, forming a yellow crust
- itchy rash
- fluid-filled blisters
If you see those symptoms, visit your health care provider. Impetigo is usually treated with topical or oral antibiotics. If you have multiple lesions or if there is an outbreak, your doctor might prescribe an oral antibiotic. There is no over-the-counter (OTC) treatment for impetigo.
Controlling and Preventing Impetigo
Untreated, impetigo often clears up on its own after a few days or weeks, Smith says. The key is to keep the infected area clean with soap and water and not to scratch it. The downside of not treating impetigo is that some people might develop more lesions that spread to other areas of their body.
And you can infect others. “To spread impetigo, you need fairly close contact — not casual contact — with the infected person or the objects they touched,” he says. Avoid spreading impetigo to other people or other parts of your body by:
- Cleaning the infected areas with soap and water.
- Loosely covering scabs and sores until they heal.
- Gently removing crusty scabs.
- Washing your hands with soap and water after touching infected areas or infected persons.
Because impetigo spreads by skin-to-skin contact, there often are small outbreaks within a family or a classroom, Smith says. Avoid touching objects that someone with impetigo has used, such as utensils, towels, sheets, clothing and toys. If you have impetigo, keep your fingernails short so the bacteria can’t live under your nails and spread. Also, don’t scratch the sores.
Call your health care provider if the symptoms don’t go away or if there are signs the infection has worsened, such as fever, pain, or increased swelling.
Is your skin swollen, red, and tender to the touch? It could be a skin infection.
If you have a skin infection, your doctor can determine if you need an antibiotic.
What are skin infections?
Skin infections occur when bacteria infect the skin and sometimes the deep tissue beneath the skin. Cellulitis is a common type of skin infection that causes redness, swelling, and pain in the infected area of the skin.
Another type of skin infection is skin abscess, which is a collection of pus under the skin.
Causes
Normally, different types of bacteria live on a person’s skin. Cellulitis or abscess can occur if there is a cut or a break in the skin that allows bacteria to enter and cause an infection.
Risk Factors
Some factors can increase the risk of cellulitis, including:
- Injury to the skin
- Skin conditions, such as athlete’s foot or eczema
- Chronic swelling of the legs or arms
- Obesity
- Diabetes
Symptoms
Symptoms of cellulitis can come on gradually or suddenly and include:
- Skin redness
- Pain, tenderness, or warmth when the affected skin is touched
- Swelling of the affected area
An abscess has similar symptoms as cellulitis but also has a collection of pus inside, which can sometimes drain out.
When to Seek Medical Care
See a doctor right away if your child is younger than 3 months old and has a fever of 100.4 °F (38 °C) or higher.
See a doctor if you have symptoms of cellulitis or abscess. Although most cases of cellulitis resolve quickly with treatment, some can spread to the lymph nodes and bloodstream and can become life-threatening.
Treatment
Your doctor will determine if you have a skin infection by asking about symptoms and doing a physical examination.
Antibiotics are needed to treat cellulitis.
If you have a skin abscess, your doctor may need to drain the pus from the abscess. Antibiotics are sometimes needed for abscesses after the pus has been drained.
Any time you take antibiotics, they can cause side effects. Side effects can range from minor issues, like a rash, to very serious health problems, such as antibiotic-resistant infections and C. diff infection, which causes diarrhea that can lead to severe colon damage and death. Call your doctor if you develop any side effects while taking your antibiotic.
In some cases, severe infections need to be treated in the hospital.
How to Feel Better
If you are prescribed antibiotics for your skin infection:
- Take them exactly as your doctor tells you.
- Do not share your antibiotics with others.
- Do not save them for later. Talk to your pharmacist about safely discarding leftover medicines.
Talk with your doctor if you have any questions about your antibiotics. Keeping the area clean is important so your skin infection can get better. If the infection is in the leg, elevating the leg can help decrease swelling.
Prevention
You can help prevent skin infections by doing the following:
- Clean your hands.
- Wash cuts with soap and water.
- Talk to your doctor about steps you can take to prevent skin infections, especially if you have a condition, such as diabetes, that increases your risk of certain skin infections.
If left untreated, this scary bacterial skin infection can be life-threatening.
Cellulitis is a bacterial infection of the skin that can cause redness, itching, pain, and swelling—and if it’s not treated promptly by a medical professional, it can become very dangerous.
“The job of the skin is to keep bad things out of your body,” says Arash Mostaghimi, MD, director of dermatology inpatient service at the Brigham and Women’s Hospital in Boston. “But if the skin’s top layer is breached, bacteria can get into the layer beneath it, and it can eventually make its way into the bloodstream.”
The inflammation and swelling associated with cellulitis isn’t the result of the bacteria itself but of the immune system’s reaction to it. “It’s your body’s efforts to fight this infection, by dilating blood vessels and recruiting white blood cells to that area” says Dr. Mostaghimi. “This can make the skin tight and red and hot, and sometimes pus can form beneath the skin, as well.”
Cellulitis can occur anywhere on the body, but it most commonly appears on the arms or legs. Doctors can usually diagnose this condition by identifying its symptoms and trademark characteristics; lab tests aren’t typically needed unless treatment has been already attempted and hasn’t worked. Once cellulitis is diagnosed, doctors usually recommend the following courses of treatment.
Oral antibiotics
The “vast majority” of cellulitis cases can be treated with a short course of oral antibiotics prescribed by a doctor—usually one to two weeks, says Dr. Mostaghimi. Cellulitis is often caused by the common bacteria Streptococci or Staphylococci, so doctors usually prescribe a broad-spectrum drug that is effective against both of these strains.
Most of the time, people start to feel better within a few days of their first antibiotic dose; their skin starts to look better, as well. But any time you take antibiotics, it’s important not to stop until your entire course is gone (or until your doctor tells you that you can stop), even if you feel better sooner. This can prevent the infection from sticking around and coming back later.
Wound cleaning and draining
Sometimes, cellulitis can cause an abscess, or a pus-filled area under the skin. If this happens, doctors will likely drain and clean the wound, then apply a covering to help the wound heal and prevent pus from leaking.
IV antibiotics
In rare cases, cellulitis doesn’t get better with oral antibiotics alone. That may be because the infection has already spread to the bloodstream and traveled throughout the body. If this happens, symptoms may include a high fever and chills, along with localized pain and swelling.
In this case, the patient may be hospitalized and IV antibiotics may be needed. People who get cellulitis on their face (called facial cellulitis) or in their eye (called orbital cellulitis) may also need IV antibiotics, according to the American Academy of Dermatology, since these types of cellulitis can be more serious and may not respond as effectively to oral antibiotics.
Cellulitis treatment at home
People who are given antibiotics to treat their cellulitis can also help their healing along by taking proper care of the affected area at home. If cellulitis occurs on an arm or a leg, for example, keeping that limb elevated can help reduce swelling and discomfort.
Over-the-counter anti-inflammatory medicines may also help relieve pain and swelling, says Dr. Mostaghimi. Doctors may recommend covering the affected area, wearing compression garments (like wraps or stockings), or using a cool, damp cloth on the affected skin.
It’s important, however, not to irritate the affected skin further, so ask your doctor about these treatments before trying them yourself. He or she can show you what types of bandages or dressings you should use, and how to clean your skin thoroughly before covering it.
Any time a person is injured or sick, getting enough rest—and practicing relaxation and stress reduction—can also be important parts of the recovery process. Research suggests that skimping on sleep and being subjected to chronic psychological stress can both be detrimental to wound healing.
Ruling out other conditions
If cellulitis isn’t getting better with antibiotics, doctors should make sure that the symptoms aren’t caused by another condition. According to Dr. Mostaghimi, other types of infections are sometimes misdiagnosed as cellulitis, which can delay proper treatment.
“Our research show that when people go to the emergency room or to their primary care doctor and the diagnosis is cellulitis, probably about a third of those cases are incorrect,” says Dr. Mostaghimi. “If you have cellulitis that doesn’t respond to treatment, or that keeps coming back in a surprising way, it may be time to check in and say, ‘Hey, maybe I don’t have this; maybe we should broaden the list of things that this could be.’”
Treating the underlying cause
Doctors don’t always know why someone gets cellulitis. Because it’s typically caused by bacteria that lives on the skin and is usually harmless, it’s not always clear why or how it gets into the body and triggers an infection.
“There are definitely times in which we get a cut or scrape or a splinter and it gets infected, and that can certainly be cellulitis,” says Dr. Mostaghimi. “But a lot of times, we see patients who suddenly got it on their leg or their arm, and we can’t identify a form of entry for the bacteria—it must be something microscopic or something very temporary.”
There are also cases of cellulitis that can be traced to skin conditions like dermatitis or athlete’s foot, which can cause tiny cracks in the skin surface and makes it vulnerable to infection. People who are obese or who have chronic illnesses (and weakened immune systems) may also be at increased risk for skin infections. In these cases, doctors should make sure that they are treating those underlying risk factors, along with the cellulitis, to make sure it does not occur again.