- 1. Aloe Vera Soothes The Rash.
- 2. Essential Oils Are An Effective Cure.
- 3. Flaxseeds Are Good For The Bones.
- 4. Hot/Cold Compression Reduces Joint Pain.
- 5. Chamomile Tea Treats Valley Fever Symptoms.
- 6. Ginger Tea Is A Natural Valley Fever Treatment.
- 7. Honey Cures The Signs Of Valley Fever.
Any person can be at risk of valley fever. The fungus causing this condition lives in dirt and travels through the air. Inhaling the contaminated air can lead to severe valley fever symptoms including joint pain, persistent cough, and fever. The condition seems familiar, but exactly what is valley fever and is there a natural treatment for it?
Also known as coccidioidomycosis, it’s a fungal infection caused by the Coccidioides fungi that multiplies in the soil and contaminates the air or dust you breathe. When you inhale the spores of the fungus, they start reproducing inside the body. A weaker immune system isn’t able to fight the fungus – leading to the fever. The disease isn’t contagious, unlike other fungal infections. However, the symptoms are discomforting.
- Fever and chills
- Muscle ache, stiffness, and pain in joints
- Night sweats
- Fatigue
- Red bumpy rashes on the upper body and legs
- Headache
- Shortness of breath and cough
- Swollen ankles, feet, and legs
- Loss of appetite
1. Aloe Vera Soothes The Rash.
Aloe vera helps restrict the development of valley fever rash. So, apply some freshly squeezed gel for 15 minutes over the affected areas thrice daily for better treatment.
2. Essential Oils Are An Effective Cure.
An essential oil blend soothes the valley fever rash. Therefore, take 3 drops of geranium and rose essential oils and mix it in half a teaspoon of coconut oil. Apply on the rashes and soothe the condition.
3. Flaxseeds Are Good For The Bones.
The seeds contain Omega-3 fatty acids that help strengthen the muscles as well as bones. So, take a teaspoon of flaxseeds every day with a glass of water.
4. Hot/Cold Compression Reduces Joint Pain.
Hot/cold compression is an instant valley fever treatment. It relaxes the muscles and reduces the pain. Heat some water or add ice as per your choice. Soak a cloth in it. Drain out the excess water from the cloth. Keep it on the joints for 15 minutes.
5. Chamomile Tea Treats Valley Fever Symptoms.
A weak immune system leads to the development of the disease. So what is a sure shot valley fever treatment? Drink chamomile tea to strengthen the immunity. In a cup of hot water, add a chamomile tea bag. Cover the tea and steep it for 5 minutes. Drink twice daily.
6. Ginger Tea Is A Natural Valley Fever Treatment.
Ginger helps in decreasing inflammation in the body. Therefore, boil a teaspoon of ginger in a cup of water. Steep the tea for 5 minutes and then strain it. Drink twice every day to get rid of the fever.
7. Honey Cures The Signs Of Valley Fever.
Honey is antimicrobial. It is effective in reducing the valley fever symptoms. Mix a teaspoon of honey in a cup of lukewarm water and drink every day. But, make sure you do not give this to infants.
Note: Articles on Ayurvedum are solely for the purpose of sharing the goodness of Ayurveda and bringing awareness on natural and healthy living. Please do not substitute it for professional medical advice. Ingredients discussed can interfere with certain medications. So, before using anything to treat yourself, always consult an Ayurveda doctor or practitioner.
Valley fever is a disease caused by the Coccidioides fungus. It thrives in dry, dusty areas particularly in the southwestern United States. It is important to know if you live in an area where the fungus tends to thrive as a huge part of prevention is knowing that you may be at risk. Those who live in Arizona, Southern California, Nevada, Utah and New Mexico are all at risk locations and even visitors can be exposed to the fungus. Thankfully it is not contagious – you cannot spread it to others nor can you get it from an infected person.
About forty percent of the people who have been infected with valley fever will never show symptoms, those that do are likely to think they have the flu. If you begin to show symptoms of skin lesions you should seek medical attention immediately – disseminated valley fever can kill you.
What are the symptoms of Valley Fever?
- Fever
- Cough
- Chest pain that varies from mild constriction to feeling like a heart attack
- Chills
- Night sweats
- Headache
- Fatigue
- Joint ache
- Red rash
- Spotty rash
- Red bumps that turn brown
- Red rash with blisters
- Red rash with pimples
If you develop the following symptoms seek medical attention immediately:
- Skin lesions
- Ulcers
- Large nodules
- Painful, swollen joints
Be sure you tell your doctor if you have been to a place where valley fever is endemic such as Arizona.
How can I prevent Valley Fever?
The best ways to prevent valley fever are common sense precautions. It is most prevalent during the summer months when it is dry.
- Wear a mask.
- Stay inside during dust storms
- Wet the soil before digging to drown spores.
- Keep doors and windows tightly closed
Dear Dr. Roach: I am a 57-year-old male who is healthy and physically fit. I contracted Valley fever last November while visiting Arizona. The initial symptoms were flulike body aches, a rash and profound night sweats that lasted for about three weeks. After returning to Canada, my family physician ordered a CT scan, which showed nodules in the left lung, the largest being 4 cm. I began to recover (untreated) before an appointment with a pulmonary specialist became available, and my doctor decided to take a wait-and-see approach. I was fully recovered and back cycling long distances in about three months.
Can I assume that this illness is behind me? I’ve met many other people who have had VF, but not one who didn’t receive some kind of antifungal. I have also read that VF can reappear years down the road. Does not having had treatment with antifungals have any influence on a recurrence?
Dr. Keith Roach (Photo: Reed Brennan)
Dear P.B.: The fungus Coccidioides is the cause of Valley fever. Coccidiomycosis, the disease caused by this fungus, is very different when it infects a young and healthy person like yourself from an infection in a person with immune system disease. You had pretty classic symptoms of Valley fever (the name for the infection in otherwise healthy people), and your body was able to overcome the infection with no treatment.
Two studies have looked at whether treatment improves symptoms faster or prevents recurrence. There was no difference between treated and untreated groups in symptoms, and no patients had recurrence of disease in the untreated group. You can be reassured that the illness is behind you.
In people taking medications to suppress the immune system (such as for auto-immune diseases) or have underlying immune system disease (advanced HIV, recent cancer chemotherapy), coccidiomycosis can be much more serious. Pregnant women need treatment as well, even with mild symptoms. Treatment in these cases is with an antifungal medicine, usually for a prolonged time, and I strongly advise treatment by a pulmonary or infectious disease specialist.
Dear Dr. Roach: Now that we are six months into the pandemic, I could use a refresher on what underlying conditions cause people to fare worse when they contract this virus. I have heard that diabetes and high blood pressure are two risk factors. Do those with controlled diabetes and high blood pressure have the same risk as uncontrolled?
Dear E.T.: Diabetes is clearly a risk for developing complications in people who are infected with SARS-CoV-2, the virus that causes COVID-19. It is likely, but not definitive, that diabetes that has not been well controlled, especially for a long time, is a much greater risk factor than well-controlled diabetes. High blood pressure is also likely a risk factor, and again, those with high blood pressure that was caught early and promptly treated with goals reached are probably less likely to have complications than those with poor control.
Other risk factors include any immune system disease or treatment (HIV, cancer, organ transplant); heart or lung disease; chronic kidney disease; sickle cell and obesity. There are many other conditions that probably increase risk. In fact, a majority of older North Americans will have at least one risk factor, which is why we all need to continue to physically distance and wear masks.
Medically reviewed by Drugs.com. Last updated on Feb 3, 2020.
- Overview
- Aftercare Instructions
- Ambulatory Care
- En Español
WHAT YOU NEED TO KNOW:
What is valley fever?
Valley fever, or coccidioidomycosis, is an infection caused by a fungus. You can get the infection if you breathe in the fungus germs. The germs are found in soil and dust in parts of the United States, Mexico, Central and South America. In the United States, most cases of valley fever occur in California, Texas, Arizona, and New Mexico.
What are the signs and symptoms of valley fever?
You may develop the following flu-like symptoms 1 to 4 weeks after you breathe in the fungus:
- Cough or trouble breathing
- Fever, chills, or night sweats
- Chest, joint, or muscle pain
- Tiredness or headache
- A rash
- Tender, swollen, red lumps on your legs
- Loss of appetite or weight loss
How is valley fever diagnosed?
Your healthcare provider will ask about your symptoms and examine you. Tell him if you have traveled recently or if you work outside. You may need any of the following tests:
- Blood tests may show the fungus that causes valley fever.
- A sample from your throat or the inside of your nose may be needed. You may need to cough mucus into a cup. A cotton swab may be used to get a sample from an open rash or wound. These are tested for the fungus that causes valley fever.
- An x-ray may show signs of infection, such as swelling and fluid around your lungs.
- A lung biopsy may be done to test for signs of a fungal infection. Lung tissue is removed and sent to a lab for tests.
How is valley fever treated?
Your symptoms usually go away on their own. It may take up to 2 months for your symptoms go away. You may need any of the following:
- NSAIDs , such as ibuprofen, help decrease swelling, pain, and fever. This medicine is available with or without a doctor’s order. NSAIDs can cause stomach bleeding or kidney problems in certain people. If you take blood thinner medicine, always ask your healthcare provider if NSAIDs are safe for you. Always read the medicine label and follow directions.
- Cough medicine may help soothe your throat and decrease your urge to cough.
How can I manage my symptoms?
- Rest as directed. Slowly start to do more each day.
- Drink liquids as directed to help prevent dehydration. Ask how much liquid to drink each day and which liquids are best for you.
- Use a cool mist humidifier to increase air moisture in your home. This may make it easier for you to breathe and help decrease your cough.
- Record the color and amount of sputum you cough up. Bring this record to your follow-up visits.
Call 911 for any of the following:
- You have severe chest pain.
- You have trouble breathing or your breathing seems faster and more shallow than usual.
- You are confused or sleepy.
When should I seek immediate care?
- Your lips or nails turn blue.
- You cough up blood.
- You have a headache, a stiff neck, and a fever.
When should I contact my healthcare provider?
- Your symptoms do not improve within 2 months.
- You have night sweats for longer than 3 weeks.
- You lose more than 10% of your weight.
- You cannot work because of your symptoms.
- Your lymph nodes are swollen.
- You have questions or concerns about your condition or care.
Care Agreement
© Copyright IBM Corporation 2020 Information is for End User’s use only and may not be sold, redistributed or otherwise used for commercial purposes. All illustrations and images included in CareNotes® are the copyrighted property of A.D.A.M., Inc. or IBM Watson Health
Further information
Always consult your healthcare provider to ensure the information displayed on this page applies to your personal circumstances.
What is pulmonary coccidioidomycosis?
Pulmonary coccidioidomycosis is an infection in the lungs caused by the fungus Coccidioides. Coccidioidomycosis is commonly called valley fever. You can get valley fever by inhaling spores from Coccidioides immitis and Coccidioides posadasii fungi. The spores are so small that you cannot see them. Valley fever fungi are commonly found in soil in the desert regions of the southwestern United States and in Central and South America.
There are two types of valley fever: acute and chronic.
Acute
Acute coccidioidomycosis is a mild form of the infection. Symptoms of the acute infection begin one to three weeks after inhaling the fungal spores and may go unnoticed. It usually goes away without treatment. Occasionally, it can disseminate into the body, causing infections in the skin, bone, heart, and central nervous system. These infections will require treatment.
Chronic
Chronic coccidioidomycosis is a long-term form of the illness. You can develop the chronic form months or years after contracting the acute form, sometimes as many as 20 years or more after the initial illness. In one form of the illness, lung abscesses (infections) can form. When the abscesses rupture, they release pus into the space between the lungs and ribs. Scarring may occur as a result.
The majority of people infected with this fungus do not develop the chronic form of pulmonary coccidioidomycosis.
You may not have any symptoms if you have the acute form of valley fever. If you do have symptoms, you may mistake them for a common cold, cough, or flu. Symptoms you may experience with the acute form include:
- cough
- loss of appetite
- fever
- shortness of breath
Symptoms of the chronic form are similar to those of tuberculosis. Symptoms you may experience with the chronic form include:
- a chronic cough
- blood-tinged sputum (coughed up mucus)
- weight loss
- wheezing
- chest pain
- muscle aches
- headache
Your doctor may perform one or more of the following tests to make a diagnosis:
- blood test to check for Coccidioides fungi in the blood
- chest X-ray to check for damage to your lungs
- culture tests on sputum (mucus you cough up from your lungs) to check for Coccidioides fungi
You most likely will not need treatment for the acute form of valley fever. Your doctor will suggest that you get plenty of rest until your symptoms go away.
If you have a weakened immune system or have the chronic form of the illness, your doctor may prescribe antifungal medications to kill the valley fever fungi. Common antifungal medications prescribed for valley fever include:
- amphotericin B
- fluconazole
- itraconazole
Rarely, for chronic valley fever, surgery is required to remove the infected or damaged parts of your lungs.
Can Valley fever be prevented?
Unfortunately, it’s hard to avoid breathing in Coccidioides fungal spores if you live in an area where they are common. While you may not be able to prevent Valley fever completely, you can take steps to reduce your risk for developing it.
- Avoid areas where you will be exposed to dirt or dust, if possible. If you must be in these areas, use an N95 respirator mask to help filter fungal spores out of the air you breathe.
- Close your windows and stay inside during dust storms.
- Avoid activities like gardening, digging, or other yard work that can expose you to fungal spores.
- Use air filters indoors.
- If you have a cut or scrape on your skin, be sure to clean the injury well with soap and water. This can help you avoid possible skin infection.
Last reviewed by a Cleveland Clinic medical professional on 03/19/2018.
References
- Centers for Disease Control and Prevention. Valley Fever. Accessed 4/11/18.
- American Association for Clinical Chemistry. Fungal Tests. Accessed 4/11/18.
- Garcia SCG, Alanis JCS, Flores JCS, et al. Coccidioidomycosis and the skin: a comprehensive review. An Bras Dermatol. 2015 Sep-Oct;90(5):610-619.
- Coccidioidomycosis. Merck Manual Consumer Version. Accessed 4/11/18.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Who gets Valley fever?
Anyone who lives in or travels to the southwestern United States (Arizona, California, Nevada, New Mexico, Texas, or Utah), or parts of Mexico or Central or South America can get Valley fever. Valley fever can affect people of any age, but it’s most common in adults aged 60 and older. Certain groups of people may be at higher risk for developing the severe forms of Valley fever, such as:
- People who have weakened immune systems, for example, people who:
- Have HIV/AIDS1
- Have had an organ transplant2
- Are taking medications such as corticosteroids or TNF-inhibitors3
- Pregnant women 4
- People who have diabetes 5
- People who are Black 5, 6 or Filipino 7
Is Valley fever contagious?
No. The fungus that causes Valley fever, Coccidioides, can’t spread from the lungs between people or between people and animals. However, in extremely rare instances, a wound infection with Coccidioides can spread Valley fever to someone else, 8 or the infection can be spread through an organ transplant with an infected organ. 9
Traveling to an endemic area
Should I worry about Valley fever if I’m traveling to an area where the fungus is common?
The risk of getting Valley fever is low when traveling to an area where Coccidioides lives in the environment, such as the southwestern United States, Mexico, or Central or South America. Your risk for infection could increase if you will be in a very dusty setting, but even then the risk is still low. If you have questions about your risk of getting Valley fever while traveling, talk to your healthcare provider. You can also consult CDC’s Travelers’ Health Yellow Book for more information.
I’ve had it before could I get it again?
Usually not. If you’ve already had Valley fever, your immune system will most likely protect you from getting it again. Some people can have the infection come back again (a relapse) after getting better the first time, but this is very rare.
Can my pets get Valley fever?
Yes. Pets, particularly dogs, can get valley fever, but it is not contagious between animals and people. Valley fever in dogs is similar to valley fever in humans. 10 Like humans, many dogs that are exposed to Coccidioides never get sick. Dogs that do develop symptoms often have symptoms that include coughing, lack of energy, and weight loss. If you’re concerned about your pet’s risk of getting Valley fever or if you think that your pet has Valley fever, please talk to a veterinarian.
Coccidioides at my workplace
What should I do if I think I’ve been exposed to Coccidioides at my workplace or in a laboratory?
If you think you’ve been exposed to Coccidioides at work or in a laboratory, you should contact your Occupational Health, Infection Control, Risk Management, or Safety/Security Department. If your workplace or laboratory doesn’t have these services, you should contact your local city, county, or state health department. Recommendations about what to do in the event of a laboratory exposure external icon have been published. 11 There is no evidence showing that antifungal medication (i.e., prophylaxis) prevents people from getting sick with Valley fever after a workplace exposure to Coccidioides. If you develop symptoms of Valley fever, contact your healthcare provider.
For more information about work-related Valley fever, please visit the CDC-NIOSH Valley fever webpage.
How can I prevent Valley fever?
It’s very difficult to avoid breathing in the fungus Coccidioides in areas where it’s common in the environment. People who live in these areas can try to avoid spending time in dusty places as much as possible. People who are at risk for severe Valley fever (such as people who have weakened immune systems, pregnant women, people who have diabetes, or people who are Black or Filipino) may be able to lower their chances of developing the infection by trying to avoid breathing in the fungal spores.
The following are some common-sense methods that may be helpful to avoid getting Valley fever. It’s important to know that although these steps are recommended, they haven’t been proven to prevent Valley fever.
- Try to avoid areas with a lot of dust like construction or excavation sites. If you can’t avoid these areas, wear an N95 respirator (a type of face mask) while you’re there.
Click for more information about respirators. - Stay inside during dust storms and close your windows.
- Avoid activities that involve close contact to dirt or dust, including yard work, gardening, and digging.
- Use air filtration measures indoors.
- Clean skin injuries well with soap and water to reduce the chances of developing a skin infection, especially if the wound was exposed to dirt or dust.
- Take preventive antifungal medication if your healthcare provider says you need it.
Is there a vaccine for Valley fever?
No. Currently, there is no vaccine to prevent Valley fever, but scientists have been trying to make one since the 1960s. Because people who’ve had Valley fever are usually protected from getting it again, a vaccine could make the body’s immune system think that it’s already had Valley fever, which would likely prevent a person from being able to get the infection.
Scientists have tried several different ways to make a Valley fever vaccine. When one version of the vaccine was tested on humans in the 1980s, it didn’t provide good protection, and it also caused people to develop side effects such as swelling at the injection site. 12 Since then, scientists have been looking at ways to make a vaccine with different ingredients that will provide better protection against Valley fever and won’t cause side effects. Studies of these new vaccines are ongoing, so it’s possible that a vaccine to prevent Valley fever could become available in the future. 13
Valley fever is a fungal lung infection that can be devastating. Learning about Valley fever can help you and your doctor recognize the symptoms early.
Valley fever is an infection caused by a fungus that lives in the soil. About 10,000 cases are reported in the United States each year, mostly from Arizona and California. Valley fever can be misdiagnosed because its symptoms are similar to those of other illnesses. Here are some important things to know about Valley fever, also called coccidioidomycosis.
From soil to lungs
The fungus that causes Valley fever, Coccidioides, is found in the southwestern United States, parts of Mexico and Central America, and parts of South America. The fungus has also been found in south-central Washington state. It probably lives in other areas in the western United States. People can get Valley fever by breathing in the microscopic fungus from the air in these areas. Valley fever does not spread from person to person.
Common symptoms may lead to delayed diagnosis
Many people who are exposed to the fungus never have symptoms. Other people may have symptoms that include:
- Fatigue (tiredness)
- Cough
- Fever
- Shortness of breath
- Headache
- Night sweats
- Muscle aches or joint pain
- Rash on upper body or legs
The symptoms of Valley fever can be similar to those of other common illnesses, which may cause delays in getting patients correctly diagnosed and treated. For many people, symptoms go away without any treatment, after weeks or months, but healthcare providers prescribe antifungal medicine for some people to try to reduce symptoms or prevent the infection from getting worse. People who have severe lung infections or infections that have spread to other parts of the body always need antifungal treatment and may need to stay in the hospital.
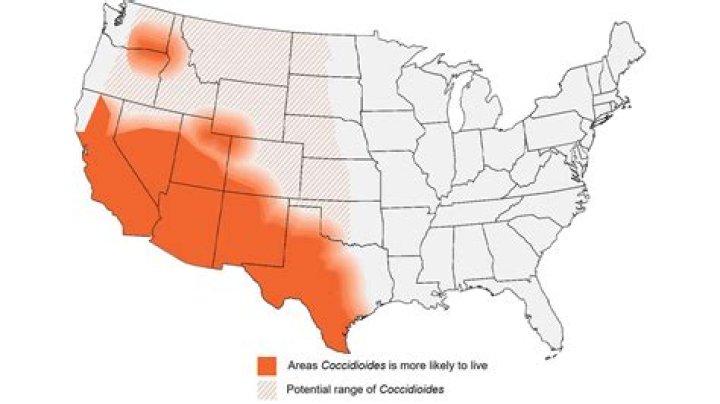
This map shows CDC’s current estimate of where the fungus that causes coccidioidomycosis (Valley fever) live in the environment in the United States. The fungus is not distributed evenly in the shaded areas, might not be present everywhere in the shaded areas, and can also be outside the shaded areas. Darker shading shows areas where Coccidioides is more likely to live. Diagonal shading shows the potential range of Coccidioides.
Estimated areas with coccidioidomycosis (Valley fever)
This map shows CDC’s current estimate of where the fungus that causes coccidioidomycosis (Valley fever) live in the environment in the United States. The fungus is not distributed evenly in the shaded areas, might not be present everywhere in the shaded areas, and can also be outside the shaded areas. Darker shading shows areas where Coccidioides is more likely to live. Diagonal shading shows the potential range of Coccidioides.
Do you have any suggestions for treating Valley Fever?
Valley Fever is an infection – usually of the lungs – caused by a fungus, Coccidioides immitis, found in the southwestern United States and northwestern Mexico. It was discovered in the San Joaquin Valley of California and is also sometimes called “San Joaquin Valley fever,” “desert fever,” or “desert rheumatism.”
Valley Fever is very common here in Arizona. We see a lot of infections in June and July and then again in October and November. In California, the “season” for Valley Fever runs from June through November. The fungus lives in the soil, and those most susceptible to infection are farm and construction workers as well as archeologists and others whose jobs involve disturbing the soil and who may inhale the spores.
More than 60 percent of all cases are so mild that those infected never feel sick and never know they have Valley Fever. Those who feel bad enough to go to the doctor usually complain of fatigue, cough, chest pain, fever, rash, headache, and joint aches. Most of the time no specific treatment is needed, just plenty of rest. However, I do suggest eating one or two cloves of raw garlic daily. Garlic has antibiotic and antifungal properties that may make it useful in counteracting fungal infections such as Valley Fever. You can make raw garlic more palatable by chopping it fine and mixing it with food. Or cut a clove into chunks and swallow them whole like pills (remember, a clove is one of the segments of a head or bulb of garlic).
About five percent of cases of Valley Fever lead to pneumonia or other breathing problems that require treatment, typically with Diflucan (fluconazole), a strong prescription antifungal drug. Side effects of this medication can include nausea, vomiting or abdominal pain, diarrhea, headache, or rash. Be sure to tell your physician about any severe or unusual side effects. In rare cases, Diflucan can cause liver damage, and before taking it women should be sure to tell their doctor if they’re pregnant or think they might be. The drug can damage the fetus although potential benefits may warrant use of the drug in pregnant women despite potential risks. In an even smaller percentage of cases of Valley Fever, the infection becomes generalized and potentially life-threatening, requiring more drastic treatment.
The best way to deal with Valley Fever would be a vaccine to prevent it. Researchers at the Valley Fever Center for Excellence here in Tucson (one of several such centers in the southwest and California) are working on a vaccine. Let’s hope they find one soon.
Dogs can bring boundless love and joy into your life. They are always there for you whether you want to play, go for a walk, or need a hug. The relationship between a dog and its owner is a beautiful thing, and in order to preserve this wonderful connection, you should be aware of potential risks and warning signs that your pup isn’t feeling well. While there are many illnesses and injuries that can threaten the health of your pet, here in Arizona one disease, in particular, should be a cause for concern: valley fever.
To protect your dog’s health, here is what every dog owner needs to know about Valley Fever symptoms and treatment.
Symptoms
Valley fever results from a fungus found in desert areas, so those of you who live in such a climate, take particular care in recognizing these symptoms. There are two different forms that this disease can take, each of which presents differently:
- Primary valley fever generally presents three weeks following initial contact with the fungus, most notably as a persistent cough. This is soon accompanied by a fever and overall decline in mood. You may notice your dog has stopped eating as well or displays a sudden lethargy or disinterest.
- Disseminated valley fever is much worse. This is the result of the disease spreading throughout your dog’s body, typically to bones and joints. When Valley Fever spreads, it causes severe pain. In extreme cases, dogs can lose the use of their legs altogether. Left untreated, it can even spread to your dog’s nervous system, a development that can often be fatal. If you haven’t already, call an emergency vet or go to your nearest emergency animal hospital as soon as you spot any signs of strange behavior or pain.
Both manifestations of valley fever are extremely dangerous to your dog’s well being, and if you suspect any of the above symptoms have presented, please do not hesitate to call your veterinarian!
Treatment
The standard protocol for treating Valley Fever depends on how far the disease has progressed. Your veterinarian will take blood samples and potentially x-rays to diagnose your pet, then decide upon the proper treatment and duration or care. Valley Fever is almost always treated through antifungal medication, and based on how far the disease has progressed, it can last anywhere from 6 months to a lifetime. The earlier you catch this disease, the shorter treatment will typically have to last.
Always be aware that your dog needs constant care alongside constant love and attention. To ensure your dog is living a happy and healthy life, always be on guard for signs of a pet emergency like Valley Fever. It’s recommended to schedule two check-ups with your veterinarian annually, but always have a local animal hospital and emergency veterinarian in mind. To help prepare you for situations like canine Valley Fever, keep an open dialogue with your veterinarian about risks and important symptoms to watch for. Dogs have a special connection with humans, and it is our duty to love and safeguard our furry best friends.
(Picture Credit: Getty Images)
Valley Fever in dogs, also known as coccidioidomycosis, is a disease caused by a fungus called Coccidioides immitis. The disease has several other names, including Desert Rheumatism, San Joaquin Valley Fever, and California Disease.
The fungus is common in the hot, dry climates of the southwestern United States, Central America, and parts of South America. Usually it stays buried in soil where it lies dormant, but when it rains, the fungus becomes active and spreads.
Anything that disturbs soil, like earthquakes or construction, can cause spores to be released from the ground, as well. When dogs breathe these spores in, they can become infected.
Many infected dogs don’t show any symptoms of Valley Fever, but some become severely ill. Dogs who suffer from Valley Fever often develop respiratory problems, and in some dogs, the disease can also be fatal.
If you see the signs of Valley Fever in your dog, you must consult your veterinarian right away so they can form a proper diagnosis and prescribe treatment. Here’s what you should know about the symptoms, causes, and treatments for Valley Fever in dogs.
Symptoms Of Valley Fever In Dogs
(Picture Credit: Getty Images)
The symptoms of Valley Fever in dogs may vary in severity, and most dogs infected by the fungus don’t show any symptoms at all. On the other hand, some dogs develop symptoms that are so serious that they become life-threatening.
Usually dogs affected by the disease show signs of respiratory illness at first and develop additional symptoms after four months or more as the disease spreads from the lungs to other parts of the body.
Here are some of the symptoms seen in dogs who suffer from Valley Fever:
- Fever
- Shortness of breath, rapid breathing, or difficulty breathing
- Coughing
- Loss of appetite
- Weakness
- Lethargy
- Diarrhea
- Vomiting
- Lameness
- Swollen joints or bones
- Swollen lymph nodes
- Neck or back pain
- Seizures
- Changes in vision
- Inflammation of the eyes
- Oozing sores on the skin
- Weight loss
- Heart failure
Causes Of Valley Fever In Dogs
(Picture Credit: Getty Images)
Valley Fever in dogs is caused by a fungus called Coccidioides immitis. Dogs who live in the hot, dry climate where this fungus is found are more at risk for exposure.
Normally the fungus is dormant underground, but rainfall, construction, crop harvests, earthquakes, or anything that disturbs the dry ground can cause spores to rise and be carried on the wind. When dogs breathe in these spores, they can become infected.
Usually dogs’ immune systems are able to fight off such infections, but dogs with compromised immune systems, including puppies and seniors, are more susceptible to developing symptoms of Valley Fever. Dogs who spend most of their time outside are also at greater risks.
Certain breeds are more predisposed to Valley Fever, including Australian Shepherds, Beagles, Boxers, Cocker Spaniels, Doberman Pinschers, Pointers, and Scottish Terriers.
Treatments For Valley Fever In Dogs
(Picture Credit: Getty Images)
Treatment for Valley Fever in dogs depends on the severity of symptoms. In most cases where symptoms are mild to moderate, dogs may need to have their physical activity limited as they recover, and they should be provided with a diet that is easily digested.
For dogs who suffer from more severe respiratory distress, oxygen therapy may be required. Other clinical signs, such as seizures, coughing, or pain, may be treated with various medications accordingly.
If the disease has spread throughout the body, then aggressive antifungal treatment may be needed. This treatment can last for six months to more than a year, even though dogs usually start to feel better within one or two weeks after the start of treatment.
It takes a long time for the infection to be completely eradicated, and in cases where the infection spreads to the central nervous system, dogs may need treatment for the rest of their lives.
Relapses are common when dog parents discontinue treatment before the infection can be completely cleared. If your dog is diagnosed with Valley Fever, it’s important that you follow your vet’s instructions fully, even if your dog seems to be feeling better.
Has your dog ever gotten sick with Valley Fever? How did your vet treat your pet? Let us know in the comments below!